
PGS/PGD

What is PGD?

Preimplantation genetic diagnosis (PGD) is a method to assess the genetic health of embryos created in an IVF cycle. After eggs are fertilized with sperm and develop into embryos with at least 8 cells, one of the cells from each embryo is removed under a microscope, and the chromosomes of that cell is analyzed to determine whether the embryo is genetically normal or not.
Who benefits from PGD?

There are a number of genetic diseases and chromosomal abnormalities that can be detected by PGD. Thus, PGD benefits patients who are carriers of genetic diseases and prevent the diseases from being expressed in their children and parents who want to avoid having chromosomal abnormalities in children. A common example of chromosomal abnormalities that can be detected by PGD is Down’s syndrome. In a more complicated process, PGD can pick up inherited genetic diseases like Tay-Sachs disease, Cystic Fibrosis, Sickle Cell disease, Huntington's Chorea disease, Cooley's Anemia, and many others.
In addition, PGD is also used in gender selection processes, where parents who want to have a child of a specific gender have only embryos of the desired gender transferred to the uterus. In contrast to gender selection methods based on sorting of sperm (between those with X chromosome and those with Y), gender selection via PGD is nearly 100% accurate.
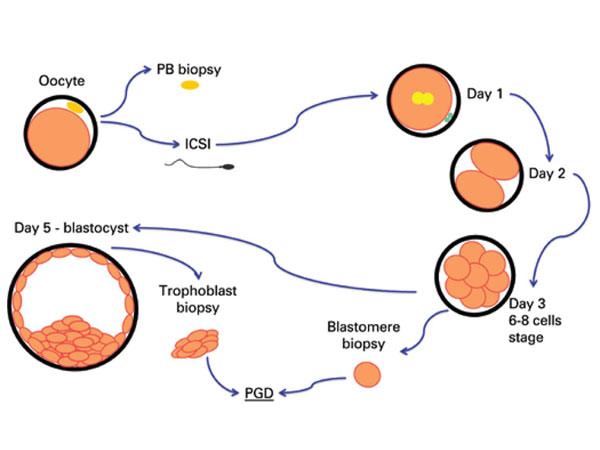

PGD at CHR

PGD became widely available during the 1990s, but it was not until 2001 that the two professional organizations in the field, American Society for Reproductive Medicine (ASRM) and Society for Assisted Reproductive Technologies (SART) issued a statement declaring the procedure no longer experimental.
In a vast majority of fertility centers, PGD is outsourced to specialized laboratories. However, at CHR, we perform PGD in-house, which ensures maximum safety of the patients' embryos and reduces the risk of problems during transit and even mix-ups.
Risk of PGD

There are several risks involved in PGD, one of which is the possibility of false positive or false negative diagnosis. Cells that make up an early-stage embryo are not all identical (this is called mosaicism). Because of mosaicism, if a biopsied cell happened to contain an abnormal chromosome that is not present in other cells, this could result in a false positive diagnosis.
Embryos also have an ability to isolate and remove some of their genetically abnormal cells, meaning that even embryos that had chromosomally abnormal cell(s) at the time of PGD may correct themselves and grow into normal babies later on.
Long-term outcomes on offspring born after PGD have not been clearly defined. In addition, removal of a cell has a chance of damaging the embryo to a degree, resulting in lower pregnancy chances compared to non-PGDed embryos.
What is PGS?

Crete Fertility Centre is one of the very few centres in Greece which perform the new method, Array-CGH (Array Comparative Genomic Hybridization) – PGS (Preimplantation Genetic Screening), with excellent results.
PGS (Preimplantation Genetic Screening) is the only method able to detect unbalanced chromosomal abnormalities. This is because balanced chromosomal abnormalities such as reciprocal translocations, inversions or ring chromosomes do not affect copy number, which is what is detected by CGH technologies. CGH enables the exploration of all 46 human chromosomes in single test and the discovery of deletions and duplications, even on microscopic scale which may lead to the identification of candidate genes to be further explored by other cytological techniques.
PGS can help in cases of advanced maternal age, multiple miscarriages and failed embryo transfers.
Humans generally have 46 chromosomes that come as 23 pairs, one of each pair from our Mum and one of each from our Dad. Problems arise when an embryo misses out on a chromosome or picks up an extra one – that’s called a chromosomal abnormality.
Chromosomal abnormalities can cause your embryo to fail to implant or miscarry or they might result in a baby born with developmental problems or a serious genetic condition.
PGS testing checks all chromosomes to see if an embryo has a balanced set, checking specifically for:
- Aneuploidy (Chromosome Abnormality): a frequent cause of unsuccessful IVF attempts, miscarriages and abnormal live births
- Translocations: looking for unbalanced parts/sets of chromosomes
- Medical Sex Selection: tells us whether the embryo is male or female which allows genetic disease risk reduction in such cases

